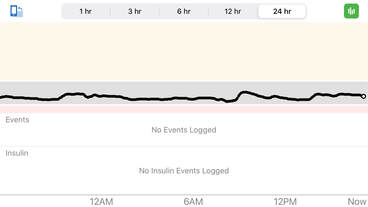
 Stable blood sugar is a beautiful thing! Stable blood sugar is a beautiful thing! For the last ten years or so I've struggled with reactive hypoglycemia related to CFRD (cystic fibrosis-related diabetes). In the last couple of years it has become very difficult to manage. Reactive hypoglycemia is a condition where the blood sugar crashes 1-3 hours after a meal containing carbohydrates, leading to distressing hypoglycemia symptoms such as shakiness, anxiety, weakness, brain fog, fatigue, tachycardia, and in severe cases, unconsciousness or even coma. Reactive hypoglycemia is more common in CFRD than many CF-specialists realize. Despite avoiding simple carbohydrates and adhering to a Paleo-ish diet for many years, my reactive hypoglycemia has only gotten worse. That is, until I started a ketogenic diet in October of 2020. I've made a remarkable improvement in my blood sugar control and I'd like to report my success in detail here.
0 Comments
 Digestive upset is a special kind of misery, and in cystic fibrosis and other digestive diseases it may be a common nuisance. Fortunately, herbal medicine is particularly effective in assisting people with these issues! All of our ancestors have been using medicinal herbs to address digestive distress for eons. Although conventional medicine has very few tools to assist us with gastrointestinal issues, especially with regards to chronic indigestion, there are many, many herbs which can help resolve GI symptoms including stomach aches, intestinal cramps, nausea, burping, constipation, loose stools and diarrhea, delayed gastric emptying, reflux, and more. In this article I will suggest a few herbs to use to address bloating and indigestion. There are so many medicinal herbs to choose from that I couldn't possibly discuss them all in one article, so I'll touch on a few that I use most frequently for myself and my clients.  Baikal skullcap Baikal skullcap Inflammation is a huge factor in the disease processes of cystic fibrosis. Some studies have shown that faulty CFTR mutations may directly result in inadequate quenching of radical oxygen species (ROS) or excessive release of other inflammatory compounds like cytokines [1,2]. In addition, our burden of chronic infection and gastrointestinal complications contribute secondary sources of inflammation. Chronic inflammation can lead to both localized and systemic issues. Localized inflammation in the lungs can lead to deficient and/or over-reactive immune responses, bronchitis, scarification and airway remodeling, allergies/asthma/hyper-reactive airway diseases, hemoptysis, pleurisy (inflammation of the pleura), and worsened infection. Localized inflammation in the gut can lead to reflux/GERD, esophagitis, gastritis, pancreatitis, gallbladder issues, liver issues, food sensitivities, malabsorption, autoimmune issues of the intestines, gut infections, general indigestion, and excessive mucus production in both the guts and the lungs (by vagal reflex). Systemic inflammation can cause insulin resistance, body pain, arthritis, achey joints and muscles, fever, fatigue, increased risk for autoimmunity, and increased risk for cardiovascular disease.  In this article, originally published in AromaCulture Magazine in July, I discuss herbal and dietary support for CF children and adults. I discuss digestion, respiratory disease, liver support, and modulation of CFTR sodium chloride channels by natural means. Cystic fibrosis is an autosomal recessive genetic disease that leads to the malfunctioning of several organ systems but most especially impacts the lungs, sinuses, and digestion. It is the most common autosomal recessive genetic disorder (meaning that each parent must be a carrier of the genetic mutation) in people of Western European decent. There are approximately 30,000 people living with cystic fibrosis (CF) in the United States, and more than 70,000 people worldwide.  For many years I've struggled with the choice of when to avoid antibiotics and what situations warrant their use. As a person with chronic lung infections related to cystic fibrosis, antibiotics have saved my life countless times, but in the last few years I've become dependent on them to function normally. Without antibiotics to control my chronic lung infections (MRSA and Pseudomonas), I often feel debilitating fatigue, get a daily fever, and cough lots and lots of mucus. While I've found many natural remedies over the years to reduce my infections, improve my immune system, and strengthen my overall health and digestion, the severity of my infections is such that I cannot avoid antibiotics completely. In general, there are no natural remedies that I know of that match the power of pharmaceutical antibiotics for use in many bacterial infections - and trust me, I've looked! As a result of my experiences both with conventional pharmaceuticals and natural medicine, my opinions about antibiotics have changed over the years. In the beginning of my healing journey and experimentation with natural medicines, I viewed antibiotics with skepticism and tried to avoid them as often as possible. I made the personal choice to suffer through many months of infection, fatigue, and heavy mucus loads in order to minimize my exposure to this class of drugs. I did this for two major reasons: minimizing the risk of developing antibiotic resistance, and mitigating the impact that excessive use of antibiotics has on the gut microbiome. For about four years, I chose to wait as long as possible between hospitalizations, and do without oral antibiotics for longer and longer periods of time. Upon reflection, I think avoiding antibiotics as often as I did was a mistake, and I wouldn't recommend people do what I did. I lost lung function during that period and developed some serious and irreversible lung damage. It's not clear whether or not this damage would have developed anyway, even if I had taken more antibiotics. I now believe that the cost-benefit analysis weighs out in favor of using antibiotics when appropriate. In the last year or so I have changed tactics and my health has benefited. Here, I will describe my experiences and review why I made these changes.  Artichoke leaf Artichoke leaf A friend of mine with CF who lives in South Africa has a history of severe gastroparesis (delayed gastric emptying) and low stomach acid, which (alongside her Crohn's, CFRD, and removal of her terminal ileum, ascending colon, and gallbladder years ago) has caused her significant digestive distress and inability to digest anything other than her extremely regimented liquid diet. For years Paula's gastroparesis has been so bad that if she doesn't eat precisely the right thing in precise quantities at precisely the right time of day, her stomach will not empty, which puts pressure on her diaphragm and lungs and can cause significant respiratory distress and vomiting. She is a great researcher and has tried many, many things to help this situation, but nothing had yet made a significant dent on these distressing symptoms (including multiple motility drugs). I've tried to strategize with Paula to figure out what was causing or had caused the issue, and secondly what do we do about it now. After a lot of trial and error, it seems we've found two things that have made a big difference in her life: lecithin and artichoke leaf (Cynara scolymus).  As a kid with CF, I was lucky in that I had heartburn rarely enough that regular use of antacids or PPIs (proton pump inhibitors) was not offered to me by my parents or doctors, so I never developed a dependence on them. But it seems such things are often suggested to CF patients as part of a standard CF routine. Due to a number of factors common in the CF lifestyle (poor diet, frequent antibiotic usage, stress, coughing, etc.) acid reflux, heartburn, and gastroesophageal reflux disease (GERD) are commonplace in the CF population. Yet mainstream medicine understands the problem entirely wrong, and so their standard treatment protocol ends up exacerbating the issue and causing more problems than you started with. I want to briefly discuss why antacids and PPIs are inappropriate for CF (and humans in general) and some alternatives to these pharmaceutical treatments for reflux.  Turmeric root, Curcuma longa Turmeric root, Curcuma longa Since about 2013, a portion of the CF community has been experimenting with "the Combo", or the combination of curcumin plus genistein supplements to help modulate CFTR function. This intervention is proving to be very helpful for many people who try it, yet we're still in the beginning stages of our experimentation. The impacts of the Combo are somewhat mutation-specific, and the rate of digestive absorption of these herbs varies person to person, thus the dose must be deduced via personal experimentation. The Combo is a simple and safe intervention with few side effects and is relatively cheap (compared to pharmaceutical CFTR modulators like Kalydeco, which cost $300,000 a year!). Both of these supplements are made up of plant constituents (genistein from soy and curcumin from turmeric root), and as you know, I'm an herbalist and a believer in the healing power of plants.  On occasion one must do strange things in the name of science. Sometimes it's necessary to challenge a few taboos to find useful information. There's hardly a body part with more taboos attached to it than the bung-hole. Oh yes, my friend. I'm going there. Let us discuss that place that our culture chooses not to think about. The "deep space" of our body. The rectum. It's a pretty useful spot. Located in between the bowel and the anus, it is of course wonderfully useful for expelling feces. And because it is a highly vascularized area of tissue, it is also very useful for absorbing things into the bloodstream. Rectal suppositories of medicine have been used for centuries, and more recently it's come to my attention that essential oils can be administered systemically via this technique.  Thyme (Thymus vulgaris) Thyme (Thymus vulgaris) For an introduction to inhaling essential oils in general, click here. In mid-May I began inhaling Benchmark Thyme essential oil in my nebulizer. For two and a half weeks I inhaled 3 drops of the oil mixed with 3mL of normal saline and nebulized it twice a day. By the end of this 2.5 week trial period I noticed a significant improvement in my lung and overall health. Of the oils I have used so far, Benchmark Thyme (BT) is probably my single favorite. In the two weeks before starting BT I was inhaling a combo of eucalyptus and tea tree oils. Although these oils kept me from declining back to pre-essential oil levels, when I began using thyme I could notice a difference. My main lung bug is MRSA, and since BT is specifically formulated to target MRSA infections, I believe this is why it has been so effective for me. |
Author
Mica (they/he) is a clinical herbalist, nutritionist, ecologist, and writer living in Abenaki territory (Vermont). *************************** Disclaimer: The content of this website and blog is for educational purposes only and should not be considered medical advice. The information provided here is not intended to replace medical care. Archives
March 2023
Categories
All
|
Photo from BotanikGuide
 RSS Feed
RSS Feed
